Initial Decline in eGFR With Dapagliflozin Not Concerning in Patients With Heart Failure and LVEF >40%
Brigham and Women’s Hospital researchers report an initial decline in estimated glomerular filtration rate (eGFR) on initiation of dapagliflozin was not associated with adverse cardiovascular or kidney outcomes and did not appear to alter the long-term trajectory of eGFR decline.
Read More...

 Targeted therapy has had much less success in treating renal cell carcinoma than in treating many other kinds of cancer. Physician-scientists at Brigham and Women’s Hospital are working on several innovative approaches to address this shortfall.
Targeted therapy has had much less success in treating renal cell carcinoma than in treating many other kinds of cancer. Physician-scientists at Brigham and Women’s Hospital are working on several innovative approaches to address this shortfall.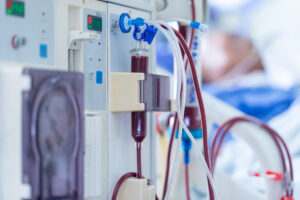
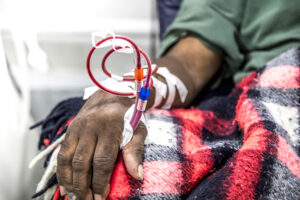
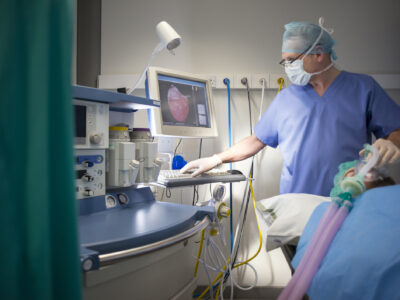
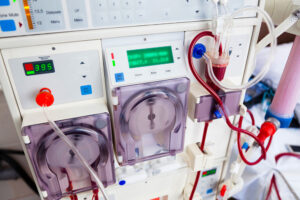 At Brigham and Women’s Hospital, nephrologists have observed an increased risk of acute kidney injury (AKI) in COVID-19 patients. Within the intensive care units (ICUs) at the Brigham, about 15 to 20 percent of COVID-19 patients have developed AKI. In some hospitals, the incidence of AKI has been reported to be as high as 25 percent.
At Brigham and Women’s Hospital, nephrologists have observed an increased risk of acute kidney injury (AKI) in COVID-19 patients. Within the intensive care units (ICUs) at the Brigham, about 15 to 20 percent of COVID-19 patients have developed AKI. In some hospitals, the incidence of AKI has been reported to be as high as 25 percent.