Preeclampsia occurs in up to 7 percent of all pregnancies and is the third-leading cause of maternal mortality around the world. Yet despite how common it is, surprisingly little is known about its underlying causes. This lack of information has made it difficult to develop methods for determining which women are most at risk of developing preeclampsia and to find ways to reduce that risk or effectively treat the condition after it develops.
A recent study led by Thomas F. McElrath, MD, PhD, an attending physician in the Division of Maternal-Fetal Medicine at Brigham and Women’s Hospital, has shown that circulating microparticle proteins (CMPs) in the blood that can be detected late in the first trimester could be used as a biomarker to predict preeclampsia risk. The research, published in Nature Scientific Reports, also revealed that the disease has at least two distinct phenotypic subtypes, depending on which pathways are activated in association with it.
“We’ve had almost 100 years of research trying to create prognostic tests and effective therapies for preeclampsia,” Dr. McElrath said. “Perhaps one of the reasons these efforts have not been as successful as we would hope is that there is actually more than one subtype of disease, and earlier studies didn’t make that distinction.”
Stratifying Disease Into Subtypes
One reason preeclampsia has been difficult to study is that this condition of pregnancy only occurs naturally in humans; there are no good animal models. In addition, preeclampsia is a disease that has been defined by its symptoms — primarily hypertension and urinary protein loss — rather than its underlying causes. The worst cases of preeclampsia can cause organ dysfunction, seizures and even death, and can lead to the need for babies to be delivered prematurely.
“Preeclampsia is a disease of the endothelium and the vascular system, but what we don’t know are the pathophysiology and the underlying causes of the symptoms that result,” Dr. McElrath said.
In the study led by Dr. McElrath, the researchers analyzed blood samples from 23 women who developed preeclampsia and ultimately delivered their babies at 35 weeks of gestation or earlier. The study also included 50 controls from healthy pregnancies. The samples had been collected at an average of 12 weeks’ gestation. They were examined for a number of different types of CMP-associated proteins.
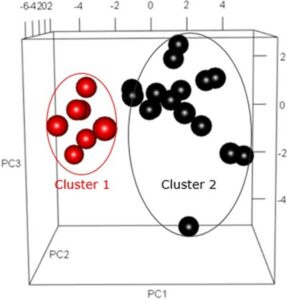
Analysis of the samples revealed two distinct clusters of CMPs that were associated with potential pathologic drivers of preeclampsia. Some cases appeared to be caused by dysfunction in platelets and clotting function, whereas others were linked to dysfunction in the immune complement system. This finding revealed that the disease has distinct subtypes. Both of these systems have been considered in the past, but interventions to target them with treatment have been unsuccessful. Dr. McElrath said this has likely been the outcome because not all cases of the disease had the same underlying cause.
“Of course, further research is needed, and it’s possible there may be more than two subtypes,” he added. “But this at least suggests a way forward, because up until now we’ve been a little bit stymied with what we’ve been able to do to help our patients.”
Developing a Model of Personalized Care
Once the findings are validated, a more immediate goal of the research is to develop prediction models for preeclampsia.
Longer term, a deeper understanding of the pathophysiology of the disease could lead to treatments targeted at these underlying causes. As with the kind of personalized treatments that are increasingly being used in oncology, these therapies would be matched with a patient’s individual subtype of disease.
“This study is the beginning of our ability to hopefully create very specific care pathways for women in pregnancy, where we could use one blood sample to determine a woman’s risk of preeclampsia,” Dr. McElrath concluded. “These findings could potentially be extended to determining risk for other conditions of pregnancy, like gestational diabetes, which would allow us to personally tailor each woman’s prenatal care.”