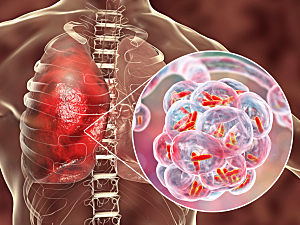
Mouse PLPP6 Regulates Allergen Sensitization
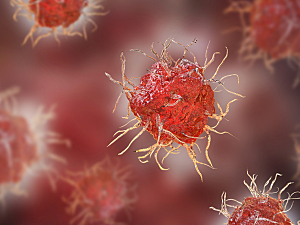
Brigham and Women’s Hospital researchers are the first to characterize Plpp6, a mouse homolog of PLPP6, as a polyisoprenyl diphosphate phosphatase that’s activated in dendritic cells after airway exposure to an aeroallergen. They suggest PLPP6 is likely a targetable regulatory checkpoint for allergic inflammation.
Read More...