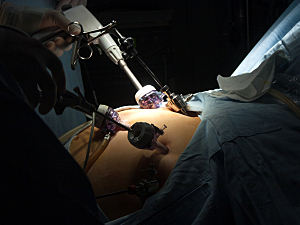
First-in-Human Trial: Ingestible Pill Accurately Monitors Respiration and Cardiac Activity
Ingestible devices have been researched since the 1950s, and proof-of-concept trials support their ability to measure pH, temperature, and gastrointestinal motility. Giovanni Traverso, MB, BChir, PhD, and colleagues have developed a vitamin-sized pill that measures respiratory rate and heart rate.
Read More...