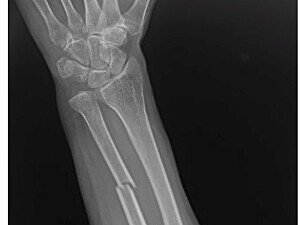
For many patients with isolated ulnar shaft fractures (IUSFs), the initial treatment is nonsurgical, particularly if the fracture has an initial displacement of <10° to 15°. However, up to about one-third of these patients eventually need surgical intervention.
Carew C. Giberson-Chen, MD, of the Harvard Combined Orthopaedic Residency Program, Brandon Earp, MD, a hand surgeon and vice chair of Clinical Operations in the Department of Orthopaedic Surgery at Brigham and Women’s Hospital, and colleagues recently explored factors associated with outcomes of IUSF nonsurgical treatment.
In the Journal of Hand Surgery, they report that patients who are currently working, have diabetes mellitus, or have an initial fracture gap ≥4 mm or initial fracture angulation >10° are at higher risk of failing nonsurgical treatment.
Methods
The study included 154 adults with IUSFs (no simultaneous ipsilateral forearm injury) initially treated nonsurgically at the Brigham or Massachusetts General Hospital between 2001 and 2020. The average patient age was 56, and 54% were female.
Any of the following outcomes were considered a failure of nonsurgical management:
- Conversion to surgical treatment
- Delayed union—Radiographs demonstrating the absence of radiographic union (defined as callus bridging at least two of the four cortices) at least three months postinjury
- Nonunion—Radiographs demonstrating the absence of radiographic union at least six months postinjury as well as persistent pain with activity and/or tenderness at the fracture site
Incidence of Failure
The average follow-up period was 4.3 months, and the average time to final follow-up radiographs was 5.3 months. 26 patients (17%) failed nonsurgical management:
- 16 delayed unions—Two patients underwent surgery with the subsequent union, and the other 14 continued nonsurgical treatments (six of those 14 were lost to follow-up before six months; the other eight achieved radiographic union without further intervention)
- Five nonunions—Three patients underwent surgery and two continued with nonsurgical treatments
- Five other conversions to surgery for pain and inability to tolerate nonsurgical treatment (n=3), inability to tolerate prolonged immobilization for nonsurgical management due to occupation (n=1) or malunion (n=1)
Risk Factors for Failure
The researchers identified radiographic thresholds associated with the failure of nonsurgical management:
- Initial fracture gap ≥4 mm—Failure in 83% of patients vs. 14% of those with a gap <4 mm
- Initial fracture angulation >15°—Failure in 50% of patients vs. 16% of those with angulation ≤15°
- Initial fracture angulation >10°—Failure in 41% of patients vs. 12% with angulation ≤10°
- Initial fracture angulation >10° but ≤15°—Failure in 38% of patients
Two patient characteristics were also noteworthy risk factors:
- Current diabetes mellitus—23% of patients who failed nonsurgical treatment vs. 8% of those who were successful
- Current employment—58% vs. 42%, respectively
Patient Counseling
The small sample in this study precluded comparative statistical analysis. Still, clinicians may wish to counsel patients with IUSF that diabetes or an initial fracture gap >4 mm may negatively affect the rate and success of their healing.
Current literature suggests IUSFs with displacement >50% or angulation >10° to 15° may benefit from operative fixation. However, this study suggests a threshold of >10° may be a more appropriate threshold for surgery.