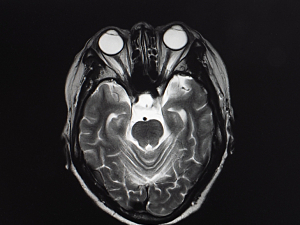
Neuromyelitis optica spectrum disorders (NMOSD) are associated with substantial healthcare utilization: emergency department (ED) visits, inpatient hospitalizations, high-dose steroids, plasma exchange, long-term treatments, neuroimaging, routine provider visits, and treatment for comorbid conditions.
Brigham and Women’s Hospital researchers recently conducted the first study of patient-reported data on the economic burden of NMOSD. Reported in Multiple Sclerosis and Related Disorders, they characterized the direct and indirect costs of relapse events (ED visits and hospitalizations). The study was led by senior author Shamik Bhattacharyya, MD, MS, an attending neurologist in Department of Neurology, former clinical fellow Kathryn B. Holroyd, MD, and Danielle Kei Pua, MD, also in the department. Colleagues and first author from Massachusetts General Hospital include Dylan R. Rice, BA, Michael Levy, MD, PhD, and Farrah J. Mateen, MD, from the Department of Neurology.
Methods
The researchers recruited for the study through NMOSD-related Facebook groups from August to September 2021. They included responses from 103 adults who completed a 20-minute online survey about the quantity and outcomes of NMOSD-attributable ED visits and hospitalizations over the past three years.
Participant Characteristics
The mean age of the respondents was 46; 85% were female, 69% were U.S. residents, 79% were white, 15% were Black, 9% were Asian, and 13% were Hispanic or Latino. The median household income was $83,000, and 48% had completed a college level of education or beyond. The average NMOSD disease duration was 3.1 years (range, <1 to 9 years).
Direct Costs
Following are the averages reported for the past three years:
- Number of ED visits: 3.6
- Number of hospital admissions (including inpatient rehabilitation stays): 1.7
- Duration of hospital admissions: 15 days
Respondents reported no out-of-pocket costs for 48% of ED visits and hospitalizations. The mean cost per event for the other 52% was $3,326.
Indirect Costs
For 26% of events, participants reported indirect costs such as childcare and housework expenses. The average cost was $1,907 per event.
Total Personal Cost
Over the past three years, the per-person cost of NMOSD was $9,201, including direct and indirect reported costs of all ED visits and hospital admissions related to NMOSD and accounting for visits in which no out-of-pocket or indirect costs were incurred.
Unquantifiable Costs
Respondents reported experiencing financial hardship in about 59% of hospitalizations. 69% of respondents said they lost income from not working because of hospital visits. Lost income could not be quantified but might represent the most significant indirect cost of NMOSD.