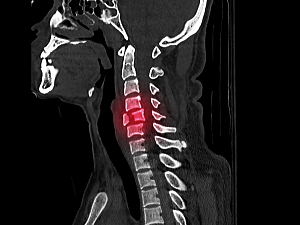
Trauma and surgery are both known to substantially increase the risk of sepsis during hospitalization. No standardized risk tool is available, though, for predicting the risk of sepsis specifically in patients who undergo vertebral fracture repair for traumatic spinal injury.
To address this knowledge gap, Hasan A. Zaidi, MD, director of spine research at the Computational Neurosciences Outcomes Center in the Department of Neurosurgery at Brigham and Women’s Hospital, and colleagues explored clinical correlates of sepsis in a large nationwide U.S. cohort. They report their findings in the Journal of Neurosurgery: Spine.
Methods
By querying the National Trauma Data Bank, the researchers generated a cohort of 29,050 adults who were hospitalized between 2011 and 2014 for vertebral fracture repair after spinal fracture and/or cord injury. 317 subjects (1.1%) developed sepsis during the hospitalization.
Risk Factors for Sepsis
Demographic and clinical characteristics significantly associated with sepsis were:
- Severe injury (Glasgow Coma Scale [GCS] score 3–8 at admission)—adjusted OR (aOR), 3.88
- GCS score 9–13 at admission—aOR, 2.71
- Spinal cord injury—aOR, 1.94
- Abdominal injury—aOR, 1.91
- Obesity—aOR, 1.86
- Diabetes mellitus—aOR, 1.53
- Male sex—aOR, 1.48
- Cervical spine fracture—aOR, 1.39
- Upper-extremity injury—aOR, 1.30
Hospital Course and Discharge
Patients who developed sepsis were significantly more likely than others to require discharge to a rehabilitative facility or discharge to home with rehabilitative support (aOR, 2.37). They were also significantly more likely to either die in a hospital or be discharged to hospice (aOR, 5.96).
Not Studied: Surgical Factors
The National Trauma Data Bank does not contain details of vertebral fracture repair, but the possibility of sepsis is influenced by the type of intervention and its invasiveness:
- If metal surgical hardware is used, its surface can become infected with gram-positive, biofilm-producing bacteria
- Longer operative time increases the chance of tissue damage, blood loss and air exposure, all of which allow invasion of microbial organisms
- Patients who have existing tissue damage around the spinal column at the time of surgery are at increased risk of surgical field infection
Clinicians should stay alert to the potential for these factors to affect the risk of post-traumatic, postoperative sepsis.