Ongoing collaboration between physicians from Massachusetts General Hospital and Brigham and Women’s Hospital has resulted in establishing the Brachial Plexus & Nerve Disorders Program at Mass General Brigham, serving patients with rare and complex upper body nerve injuries and neuromuscular conditions.
“Establishing this program provides a treatment option for patients that previously had few avenues for care,” says Dafang Zhang, MD, co-director of the Program. “Although rare, these injuries require accurate diagnosis and thoughtful intervention to avoid devastating long-term consequences.”
Complex Injuries With Far-reaching Effects
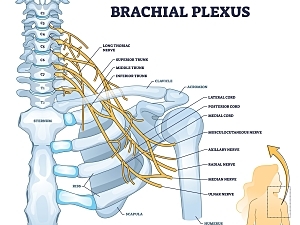
The brachial plexus comprises an interwoven network of nerves that branch out from the neck through the upper torso and shoulders. These nerves connect to those in the arms and control motion and feeling in the wrist, hand, and arm. As a result, common symptoms associated with brachial plexus injuries (BPIs) include:
- Numbness or loss of feeling in the hand or arm
- Loss of control or movement in the shoulder, arm, wrist, or hand
- A burning sensation or sharp pain in the shoulder or arm
BPIs are generally described according to the severity and type of trauma:
- Neuropraxia: Stretching of nerves to the point of injury (compression or traction)
- Rupture: Stretching that results in either a partial or complete tear in the nerve
- Neuroma: Complications from scar tissue formed during the repair of an injured nerve
- Neuritis (Parsonage Turner syndrome): A disorder that progresses from shoulder and upper arm pain to weakness, muscle loss, and the loss of sensation
- Avulsion: Complete separation of the nerve from the spinal cord resulting in permanent weakness and loss of feeling
Obstetric BPIs are relatively common (up to 3 injuries per 1,000 births) based on the vulnerability of the head and neck and the positioning of the baby during birth.
For adults, BPIs can be non-traumatic or traumatic, with the latter broadly categorized as resulting from the following:
- Blunt trauma
- Athletic injuries
- Gunshot wounds
- Medical trauma
- Cancer
- Radiation therapy
Dr. Zhang explains that in some cases, these injuries can heal themselves over time. However, recognizing the differences between injury types is key to an accurate diagnosis. “Diagnosis of non-traumatic brachial plexus disorders can be particularly difficult, given the inclination to assign other more common indications, such as a herniated disc or carpal tunnel syndrome, as the cause.”
On the other hand, traumatic BPIs are frequently accompanied by other traumas that complicate the diagnosis of something already difficult to identify. “These injuries are frequently associated with motorcycle and other motor vehicle accidents and tend to disproportionately affect a younger male demographic,” says Dr. Zhang. “In traumatic BPIs that requires surgical intervention, time to treatment is a crucial factor in determining long-term outcomes for the patient.”
Meeting a Critical Need for Specialized Care
A primary motivating factor for establishing the program originated from findings published in the Journal of Hand Surgery demonstrating the high prevalence of, and factors associated with, delayed referrals to a brachial plexus surgeon. The time threshold for the study was based on a previous report in the Journal of Neurosurgery indicating optimal outcomes for BPI interventions were within three months after the injury.
These interventions involve surgery to repair the damage, and can include the following:
- Nerve repair to reconnect torn nerves
- Neurolysis to remove scar tissue from injured nerves
- Nerve grafting using a healthy nerve from the patient to connect the ends of a separated nerve
- Nerve transfer to attach a functional nerve to the injured nerve to promote new growth
- Tendon/muscle transfer from another region to the affected area to restore function
“Our findings showed that nearly 50% of patients within relatively close proximity to two hospitals capable of treating BPIs experienced delayed referrals, meaning more than three months from injury,” explains Dr. Zhang. “The takeaways were the need to establish additional multidisciplinary centers specializing in BPIs and increase outreach to local and regional hospitals to improve the timeliness of referrals.”
What followed was a confluence of events that brought together the right people at the right time and place to establish one of these centers at Mass General Brigham. Two of the program co-directors bring a wealth of experience rare in such a specialty at a single institution. Dr. Zhang explains that he and his co-director, Rohit Garg, MBBS, trained extensively in Thailand and India, both locations with notoriously high rates of traffic-related injuries and corresponding elevated incidences of BPIs.
“These countries have historically led the world in BPIs, and so their local expertise was born out of necessity,” says Dr. Zhang. “As a result, training in these places was some of the best preparation possible for what we are doing here in New England.”
Additionally, Dr. Zhang acknowledges his other co-director, Bassem Elhassan, MD, as an enormous asset to the program. “Dr. Elhassan is an international expert in shoulder procedures, especially those involving joint fusion and tendon transfer.”
The result is that patients benefit from evaluation by clinicians with extensive experience in diagnosing and treating highly complex injuries. “More than one of us is generally present throughout the evaluation process,” says Dr. Zhang. “From the standpoint of both the patient and physician, it is extraordinarily beneficial to be surrounded by experts committed to ensuring the best care possible.”
The Right Place at the Right Time
The Brachial Plexus & Nerve Disorders Program began as a shared interest between three surgeons. Its inception was fostered by the arrival of Dr. Elhassan from the Mayo Clinic at an opportune time. However, making the program successful has required a larger team effort.
“Our ability to stand up this collaboration is a direct result of the amazing infrastructure and support provided by the Mass General Brigham network and especially the motivation our colleagues show,” says Dr. Zhang.
In situations requiring specialized experience in a particular area, surgeons from across different divisions and disciplines have been consistently willing to provide their expertise to guarantee the best outcomes for the patients.
“Our goal was to establish a program capable of timely and accurate evaluation, and treatment of patients with these unique injuries,” says Dr. Zhang. “Having done this, we want to emphasize that there are no problems in these areas too big or small for referral.”
Patients and referring physicians can contact Dr. Zhang and the program team via email at brachialplexus@partners.org or through an appointment request form on their website.