Researchers from Brigham and Women’s Hospital and the Massachusetts Institute of Technology (MIT) have developed a new way to deliver drugs and modulate nutrition through a synthetic coating in the small intestine. A proof-of-concept study for the gastrointestinal synthetic epithelial linings (GSEL) system was conducted under grants from the Bill and Melinda Gates Foundation and the National Institutes of Health, and results were published in Science Translational Medicine.
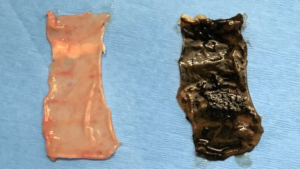
GSEL is delivered via a dopamine-based solution that reacts with the enzyme catalase in the epithelial tissues lining the small intestine, where it coats the tissue and polymerizes. Once polymerized, the coating remains stable for up to 24 hours, allowing drugs to be delivered in a more sustained way. This delivery model could reduce drug treatments from multiple doses a day to just one.
Assembling Molecules of Dopamine Into the Polymer
According to the study’s first author, Brigham and MIT biomedical scientist Junwei Li, the research team discovered that an enzyme called catalase could help assemble molecules of dopamine into the polymer (poly-dopamine). These polymers have muco-adhesion properties, which means that after polymerization, the polymer can attach to the tissue very strongly. Also, catalase is found throughout the digestive tract, with especially high levels in the upper region of the small intestine.
“This is the first example, to the best of our knowledge, of a small intestinal targeting system enabled through in-situ tissue-enzyme-catalyzed polymerization,” Li said. “Very few people would think about how you can make a polymer inside your body by your own enzyme or your own molecular chemical like dopamine.”
C. Giovanni Traverso, MB, BChir, PhD, a gastroenterologist and biomedical engineer in the Brigham’s Division of Gastroenterology, Hepatology and Endoscopy, is a member of the Brigham/MIT team that developed the system. He said the initial motivation for the effort was to improve the administration of medication in children.
“As a father of young children, I know how difficult it can be for them to take tablet- and capsule-based medications, as the possibility of choking is high,” he said. “The novel liquid solution solves that problem and provides extended release that makes it easier for both children and adults to adhere to medication protocols.”
Proof of Concept Demonstrated
The research team tested the system’s proof of concept in pig models by endoscopically delivering a solution-encapsulated form of praziquantel, a drug that treats parasitic infections such as schistosomiasis. In the study, the solution showed enhanced intestinal drug retention and adsorption.
“Praziquantel is a challenging drug to administer in pill form,” Dr. Traverso said. “The pills are large, have a bad taste and need to be taken two to three times a day. GSEL provides a mechanism to deliver the drugs in a liquid form that would be more appealing to patients.”
Modifying the GSEL system into an ingestible form and testing the effects of chronic use are the team’s next challenges and are crucial steps in moving from pig models to human trials, Dr. Traverso noted.
Potential Application in Nutrition and Metabolic Disease
The GSEL system’s ability to improve lactose digestion and regulate glucose absorption also has potential applications for treating metabolic conditions such as lactose intolerance, diabetes and obesity.
“The transient, semi-permeable barrier it forms can help modulate nutrition to treat metabolic disease, and its enzymatic immobilization enhances digestive supplementation,” Dr. Traverso said. “GSEL therefore holds the promise for new tools we can use in the fight against society’s obesity epidemic.”
Dr. Traverso’s long-term goal is for the GSEL system to be commercially developed to provide solutions for patients across a range of conditions globally, including the treatment of infectious disease in children, metabolic disease and gastrointestinal disorders.
Developing Solutions for Major Challenges
The GSEL system project does not mark the first time Dr. Traverso and his colleagues at the Brigham and MIT have worked with the Gates Foundation on new systems for oral drug delivery.
Several years ago, their team tackled a medication adherence project by developing oral capsules that open up like stars with arms that span over the opening of the pylorus, allowing them to stay in the stomach for multiple days, weeks or even months. Dr. Traverso’s team has applied these systems for the treatment of HIV and malaria and as a monthly oral contraceptive. He added that those systems are now in commercial development and undergoing Phase 1 and 2 trials across a range of indications.
According to Dr. Traverso, the work conducted in his laboratories at the Brigham and MIT is highly translational and a testament to the team’s blend of clinical and fundamental engineering expertise. “We’re uniquely situated to move swiftly in developing solutions that can be applied to significant health challenges,” he concluded.