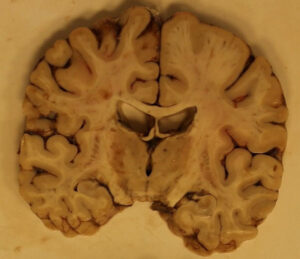
While COVID-19 primarily affects the lungs of those infected, many patients have reported a wide range of unusual neurological symptoms. These include headaches, altered mental status, strokes, seizures and loss of smell. Many researchers have hoped that autopsies could shed light on the unknowns of COVID-19, caused by the novel coronavirus SARS-CoV-2.
The New England Journal of Medicine (NEJM) recently published a letter to the editor that reported findings from 18 autopsies of COVID-19 patients who died in April, 2020. With the help of the autopsy, histology, and neuropathology technical staff, pathologists at Brigham and Women’s Hospital analyzed samples from ten major areas of the brains. The team focused on the olfactory tract and brainstem due to the possible involvement of these areas in neurological symptoms. The clinical aspects of the patients’ histories were examined by the Brigham’s Pathology team in collaboration with neurologists at the Brigham and Massachusetts General Hospital (MGH). The Broad Institute helped perform the molecular testing.
“Our findings showed high levels of hypoxic-ischemic injury, which is to be expected in patients with severe lung disease,” says Isaac Solomon, MD, PhD, a pathologist in the Brigham’s Department of Pathology. While the hypoxic-ischemic injury—caused by oxygen deprivation to the brain—isn’t surprising, the authors found similar injury between patients with long intensive care unit (ICU) admissions and those who died shortly after presentation. This raises questions about the potential for brain damage caused by mild or even asymptomatic cases of COVID-19.
Additionally, analysis of the brain sections from the 18 deceased patients didn’t show any evidence of direct viral infection, and only minimal inflammation in the brain. This suggests that SARS-CoV-2 isn’t entering the brain, which has positive implications for treatment options.
Autopsies Show Hypoxia, Not Encephalitis
When the brain is deprived of oxygen for an extended period of time, neurons begin to die, which tends to be most evident in the hippocampus, cerebellum and cerebral cortex. Pathologists observed neuronal death in these brain areas of all 18 patients. But there wasn’t any evidence of encephalitis, or acute inflammation in the brain, which is typically seen in arboviruses, human immunodeficiency virus (HIV), and herpes simplex virus (HSV-1).
“We didn’t see any histological evidence of the virus,” says Dr. Solomon. “With viral encephalitis, we typically see a plethora of lymphocytes and microglia, which destroy virus-infected neurons, but we didn’t see anything like that.”
To examine viral RNA, the team used quantitative reverse transcription polymerase chain reaction, or qRT-PCR. They observed about a million times less copies of viral RNA in the brain compared to the lungs of the same patients. Although there were some copies of viral RNA detected in the brain, it was unclear whether this represented intact virions (an entire virus particle) infecting brain tissue, or viral RNA circulating through the blood within the cerebral vasculature.
Dr. Solomon adds that the team didn’t observe any microhemorrhages, microthrombi or demyelination, which have been reported in other studies. This could be due to either the rarity of these findings or differences in premortem clinical and treatment courses.
Lack of Encephalitis Suggests Virus Does Not Enter the Brain
Previously, researchers have hypothesized that the coronavirus might enter the brain via the olfactory tract or the blood. This study found no evidence of damage or inflammation in the olfactory tract. If the virus spreads hematogenously (through the bloodstream), it doesn’t do so to any great effect. This could be due to an inability to cross the blood-brain barrier, or because the immune system is able to neutralize the amount of SARS-CoV-2 that reaches the brain.
Either way, this finding has positive implications for treatment development. “If we know that the virus doesn’t enter the brain, then we don’t have to worry about whether the drugs we use to treat the virus can enter the brain,” says Dr. Solomon. This is helpful information for vaccine development as well, for the same reason.
Another takeaway from the 18 autopsies concerns the extent of hypoxic-ischemic injury. Neuronal death is irreversible, so this damage is permanent even in recovered patients. Dr. Solomon believes this fact highlights the importance of treating other organs besides the brain in order to preserve brain function.
“From a physiological perspective, there are good reasons for the neurological symptoms, which is organ damage,” says Dr. Solomon. “The best way to treat the hypoxic injury to the brain isn’t by treating the brain, but by treating the lungs to increase the brain’s supply of oxygenated blood.”
Damage to Neurons May Affect Recovered COVID-19 Patients
It’s difficult to determine when exactly the 18 patients were infected, but death ranged from the same day as onset of symptoms to 32 days after onset. This means some patients died quickly, while others were in long-term intensive care.
“While the hypoxic-ischemic injury was more severe in some than others, all of them had some level of injury to the brain,” says Dr. Solomon. Because all 18 COVID-19 cases were fatal, they represent the extreme end of damage. Even so, “people who weren’t hospitalized and didn’t die are likely having some loss of neurons as well, depending on how severe their case was.”
The pattern of hypoxia poses the potential for long-term damage in patients who survive COVID-19. “Even people who are asymptomatic may experience long-lasting damage to the brain,” says Dr. Solomon.
It’s unclear how this damage might manifest over time, but Dr. Solomon thinks that it could accelerate aging of the brain. “The more subtle the effects, the longer it’ll take us to recognize,” he says. “It’s hard to spot mild cognitive deficits that are occurring prematurely.”
Studies to this effect could be performed on recovered COVID-19 patients with the help of MRI techniques and longitudinal cognitive testing. For now, the focus continues to be treatment and vaccine development. Since the letter’s publication, Dr. Solomon and his team have examined 15 more autopsies, which show similar findings to the first 18.