Can insulin be given to patients without injection through the skin? This is the problem that Brigham and Women’s gastroenterologist, C. Giovanni Traverso, MD, PhD, is trying to solve. Daily injections require training and can be painful for patients living with diabetes. As a result, physicians may hesitate to prescribe insulin for years—despite its immense therapeutic value—selecting alternatives that may not work as well but which can be taken orally instead.
A method for oral insulin delivery has long been desired by patients and physicians alike; however, the size of the insulin molecule itself creates a challenge for traditional oral delivery. Unlike the plethora of oral medications that can remain intact despite the gastrointestinal assault of stomach acidity and protein-catalyzing enzymes, biomacromolecules like insulin cannot withstand the voyage of oral drug delivery without degrading. Moreover, the diffusion of macromolecules through stomach tissue is too slow to be therapeutically effective. To address this unique medical challenge, Dr. Traverso and his collaborators have invented a new oral drug delivery system for biomacromolecules that could help revolutionize not only diabetes treatment, but the administration of other medicines requiring injection. Their research was recently published in Science.
The Leopard Tortoise: Natural Inspiration for a New Medical Device
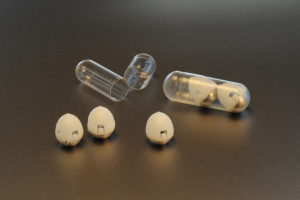
The researchers’ invention is an ingestible, self-orienting millimeter-scale applicator (SOMA) modeled after the leopard tortoise and weeble wobble toys, both of which have the capacity to self-orient. The leopard tortoise is a species which, by design, has a highly curved upper shell that enables it to redirect itself into an upright position. Additionally, the structure of the tortoise’s lower shell creates stability. Recognizing the need to have the device properly positioned, the research team looked to nature for inspiration and ultimately designed the SOMA to closely mirror the shape of the leopard-tortoise shell, lending it the same self-orienting properties. As a result, the device, which contains a microneedle made from compressed powdered insulin, always aims toward the stomach lining. The design also incorporates safety considerations. Dr. Traverso explains: “Whenever one thinks about ingestible devices, one of the key things we think about is safety. We wanted it to pass through the gastrointestinal tract safely, so we designed this system to be the size of a blueberry.”
When deciding upon the site of the injection, the stomach was determined to be a superior injection site for the microneedle compared to the small intestine, due to the relative thickness of the stomach lining and its corresponding decrease in perforation risk. Additionally, delivering medication through the stomach ensures rapid and consistent delivery across different people.
The microneedle-loaded ingestible device is theoretically painless, though human trials will address this question further. Dr. Traverso explains that pain receptors akin to the ones on skin are not present in the area of the stomach where the oral device delivers the insulin. The question remains as to how injecting insulin or other medicine via the stomach on a regular basis would impact the quality of the stomach lining, which will require further research.
The Value of a Multidisciplinary Team Approach
Dr. Traverso describes the research collaboration that led to this breakthrough treatment delivery device as an example of academic and industry cooperation that was very successful, citing their multi-institutional collaboration with MIT and Novo Nordisk. He additionally credits their success to multidisciplinary teamwork, noting that their group was comprised of individuals with highly varied backgrounds, ranging from engineering to medicine to pharmacology. “It’s a fairly diverse group of scientists coming together around a major challenge. There’s a really broad set of expertise represented,” he notes. “This is an example of how multidisciplinary teams can have a tremendous impact in developing solutions to major challenges. The major challenge we are addressing is how to administer biologics orally. It takes scientists with many different backgrounds working together to realize these types of solutions.”
A Wide Range of Applications for Patient Care
The SOMA could have a much wider use case than insulin delivery; people with a variety of health conditions may benefit from this new drug delivery method in the future. Dr. Traverso envisions a day in which a wide variety of biologics could be administered orally. Antibodies could be delivered this way. Or routine vaccinations, if the device was loaded with antigens. The team is also exploring the delivery of DNA and RNA – nucleic acids – as a potentially good use case for this invention.