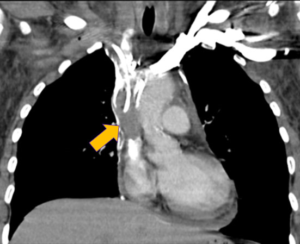
Today’s cancer therapies are helping patients live longer. However, treatments including surgery, radiation, chemotherapy and certain targeted and immunological therapies increase the risk of developing cancer-associated thrombosis (CAT). Physicians at Brigham and Women’s Hospital’s Heart & Vascular Center are working with colleagues at Dana-Farber Cancer Institute (DFCI) to help prevent CAT and minimize its effect on timely cancer care.
“Venous thromboembolism has become a major cause of morbidity and mortality in patients with cancer,” said Gregory Piazza, MD, MS, director of vascular medicine at the Brigham’s Division of Cardiovascular Medicine. “Often, it can delay cancer treatment by making patients ineligible to start or continue their therapy while the thrombosis is addressed.”
Dr. Piazza added that tumors can grow and advance during thromboembolism treatment, making the waiting period particularly concerning. “We need to make sure that a patient’s cancer care is not impeded or challenged by a thromboembolism and that they get back to their cancer therapy as quickly as possible,” he said.
CAT Guidelines Provide Varied Viewpoints
As part of his research on CAT, Dr. Piazza recently conducted a review of evidence-based guidelines for managing the condition. The review, published in The Oncologist, showed that for most clinical topics, the different guidelines offer roughly similar management advice. However, he explained, they address the issue from different viewpoints.
“It might be nice to have one universal guideline that everyone turns to, but that’s probably not realistic,” Dr. Piazza said. “Having multiple guidelines reflects the complex and multidisciplinary nature of caring for patients with CAT. Clinicians can benefit from the varied perspectives that each specialty brings and get a much more well-rounded view of the issue.”
The review, wrote its authors, should “serve as a catalyst for further research … on optimal diagnostic, preventive and management strategies for CAT, and provide comprehensive advice on these topics for the busy practitioner.”
Identifying and Treating High-Risk Patients
One of the next important steps in CAT management, Dr. Piazza said, is creating systems to spot patients who are at increased risk for developing thrombosis while undergoing cancer therapy. He wants to find biological markers that flag cancer patients who need preventive care. In addition, he is researching a novel testing protocol involving activated coagulation in patients who have not yet had a thrombosis episode.
“If we can identify these high-risk patients, then we can look at intervening with a low dose of anti-coagulant treatment that would prevent CAT without derailing their cancer care,” he said. “It is much easier to prevent thrombosis with a lower dose than to treat it with a higher dose.”
Dr. Piazza noted that the insights uncovered in his review of CAT guidelines has shifted the way he and his colleagues at DFCI care for cancer patients. “I’ve started thinking about and addressing CAT risks at an earlier point in the patient care continuum,” he said. “And I’m benefitting from the diverse range of expert voices to give me new perspectives I may not have considered before.”
As an example, Dr. Piazza said he now looks for ways to integrate data on using direct oral anti-coagulants instead of injectable anti-coagulants. “Injectables have been used for decades, but daily self-injections place a significant burden on patients,” he said. “With safe and effective oral therapies, we can make our patients’ lives easier.”
Leadership in Cardio-Oncology
The field of cardio-oncology — understanding and treating cardiovascular disease in all its forms for patients with cancer — is a rapidly growing one. The combined Cardio-oncology Program at Dana-Farber/Brigham and Women’s Cancer Center (DF/BWCC) is well-equipped to manage patients with a wide range of conditions.
“My colleagues and I handle complicated patients with conditions ranging from cardiac complications, such as heart failure and pericardial disease, to vascular complications such as thromboembolism, aneurysm and inflammation or narrowing of the blood vessels,” said Anju Nohria, MD, MsC, director of cardio-oncology at DF/BWCC.
Effectively managing CAT requires the close collaboration of oncologists and cardiovascular specialists, according to Umberto Campia, MD, cardiologist and vascular medicine specialist.
“The Cardio-oncology Program brings together the expertise of different specialties in a truly multidisciplinary approach, optimizing management of complex clinical scenarios and of cardiovascular complications of cancer treatments such as CAT,” Dr. Campia explained. “Our next frontier is to identify predictors of CAT and implement a prophylactic strategy to allow the delivery of the most effective cancer treatments with the lowest risk of side effects and adverse events.”
“Our Heart and Vascular Center team brings together expertise in cardiac and vascular care to focus on complications of cancer and cancer-directed therapy,” Dr. Piazza concluded. “With our colleagues at DFCI, we’re in an excellent position to provide superior care for a large population of patients who are in various stages of treatment for cancer.”