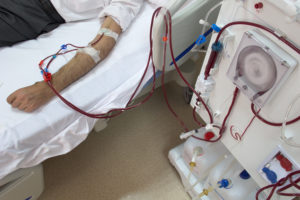
Brigham and Women’s Hospital has been on the forefront of nephrology for decades: in 1954, the hospital was the site of the first successful living-donor kidney transplant. Today, the Brigham continues its legacy of innovation in kidney dialysis research and care through its Interventional Nephrology service at Brigham and Women’s Faulkner Hospital, one of the few programs of its kind in the country.
Established to help the growing number of patients facing dialysis—an estimated 10,820 in Massachusetts alone—interventional nephrology focuses on managing and maintaining dialysis vascular access as well as placing and replacing catheters that provide circulatory-system access. It uses a range of specialized imaging and other diagnostic techniques to evaluate blood flow, vessel anatomy, blood pressure in the dialysis access and possible blockages in the flow circuit.
Before the advent of interventional nephrology, dialysis access care was often delegated to a variety of specialists with other primary clinical foci, which led to delays in diagnosis and treatment. Frequent complications, such as fistula or graft stenosis, thrombosis and central vein occlusions, were often associated with hospital admissions, waiting for a procedure room and operator availability, further delaying dialysis treatments.
“The Brigham established the program in 2008 to address these gaps in clinical care,” said Dirk M. Hentschel, MD, director of Interventional Nephrology. “We prioritize dialysis patients, often providing same-day service, which results in standardized, timely care and reduced hospital admissions.”
Nephrologists in the Brigham’s Interventional Nephrology department work collaboratively with vascular surgeons and transplant surgeons. It has become so successful that it is now a regional referral center for more than 45 dialysis units throughout New England, conducting more than 2,000 procedures a year.
“The Brigham has become well-known for taking on the most challenging patients,” Dr. Hentschel said.
Part of the service’s reputation can be traced to its 80 percent maturation rates for forearm fistulas, a procedure that has a up to a 70 percent failure rate nationwide.
“We emphasize forearm fistulas over upper arm fistulas because they last longer, have a lower chance of steal syndrome and lower rates of aneurysm formation and result in less injury and stress on the body as a whole due to overall lower fistula blood flow,” Dr. Hentschel said. “With upper arm fistulas, we focus on controlling access flow by using the radial artery instead of the brachial artery, which leads to fewer complications.”
According to Dr. Hentschel, the use of forearm fistulas is one example of how the Brigham is studying and standardizing new patterns of dialysis care. He and his colleagues are working on several research studies to further define how patient care is delivered.
For example, Florian Toegel, MD, PhD, one of three physicians to complete an interventional nephrology fellowship at the Brigham, received an award from the American Society of Diagnostic and Interventional Nephrology for his research on reducing flow and the number of interventions when treating vein stenoses in the cephalic arch. His research uncovered a correlation between the angulation of the cephalic arch and how long stent grafts maintain their patency.
Adina S. Voiculescu, MD, the first physician to complete an interventional nephrology fellowship at the Brigham, received an award from the American Society of Diagnostic and Intervention for her research on disrupting dialysis catheter fibrinous sheaths to enhance treatment of catheter-associated bacteremia.
In other research, Patrick K. McGlynn, MD, also a Brigham Fellow, recently published a study that looked at how to better create forearm fistula access by conducting ultrasounds in the OR after anesthesia. This approach uses the relaxing effects of the anesthesia on vessels to see other options in the forearm in addition to those identified in regular ultrasounds.
Dr. Hentschel and his colleagues also are working closely with Brigham’s Nephrology Transplant group to address the ongoing health of patients who receive kidney transplants by managing the cardiovascular implications of long-term, high-flow fistulas. In addition, his group is working with surgeons on peritoneal catheter placement and maintenance.
“One of the Brigham’s goals is to increase the number of patients who can receive treatment at home, and peritoneal dialysis is key to that effort,” he concluded.