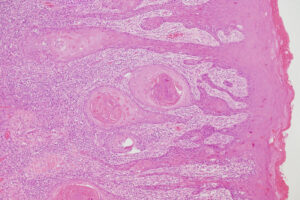
Researchers at Dana-Farber/Brigham and Women’s Cancer Center (DF/BWCC) are advancing innovative approaches to decrease tumor recurrence rates in patients with HPV-negative squamous cell carcinoma of the head and neck (SCCHN).
The new approach, detailed in Phase 2 trials published in Clinical Cancer Research and JAMA Oncology, involves administering neoadjuvant immunotherapy, including pembrolizumab (in the Clinical Cancer Research study) and nivolumab or nivolumab plus ipilimumab (in the JAMA Oncology study), prior to surgery for SCCHN.
“Recurrence rates among patients with advanced HPV-negative head and neck cancer can be up to 40–50 percent after the definitive treatment consisting of surgery, chemotherapy and radiation,” said Ravindra Uppaluri, MD, PhD, chief of head and neck surgical oncology at Brigham and Women’s Hospital and lead author of the Clinical Cancer Research study. “Once tumors come back, a vast majority of these patients will die from their recurrences.”
Dr. Uppaluri and his DF/BWCC colleagues aim to improve on those outcomes by studying the potential neoadjuvant therapeutic benefits of these programmed cell death protein 1 inhibitors. Those benefits may include:
- Reducing the extent of surgery and intensity of adjuvant therapy by tumor downstaging
- Reducing the risk of distant metastatic spread by early introduction of systemic therapy
- Converting unresectable to resectable disease
- Evaluating tumor response biomarkers
“Much of the excitement in immunotherapy has been aimed at improving treatments once the cancer has recurred and/or spread to distant organs,” Dr. Uppaluri said. “This new work focuses on introducing immunotherapy to improve outcomes in the definitive setting, when tumors first present.”
Neoadjuvant Pembrolizumab Proven Safe and Effective
Dr. Uppaluri co-led the multicenter, Phase 2 trial of neoadjuvant pembrolizumab, which was the first study to ask whether neoadjuvant and adjuvant immunotherapy would be safe and improve patient survival. This trial was started with Douglas R. Adkins, MD, at Washington University in St. Louis, and the collaboration extended to DF/BWCC.
In the trial, patients received a single 200 mg dose of neoadjuvant pembrolizumab. Two to three weeks later, patients underwent surgical tumor ablation. Patients then received postoperative adjuvant treatment as dictated by the tumor pathology. In addition, those patients with high-risk pathology received adjuvant pembrolizumab.
The surprising finding early in this study was a positive pathological response to the neoadjuvant treatment, which in the final analysis was observed in 44 percent of the patients. Tumor downstaging was observed in 19 percent of patients, with one exceptional responder starting out with Stage 4 disease and ending with Stage 1 disease after a single dose of pembrolizumab.
Although the trial was small and did not have a control arm, the one-year relapse rate in patients with high-risk pathology was lower than historical levels. No adverse events or unexpected surgical delays or complications occurred. The study also defined pathological and genomic biomarkers of response and potential for clinical impact.
“The approach was found to be safe in the surgical setting,” Dr. Upplauri said. “The positive pathological response suggests an activated immune response, which may make a significant difference in patient outcomes. Moreover, identification of biomarkers places us closer to identifying patients who will respond to this drug and understanding why patients respond the way they do.”
According to Dr. Uppaluri, this small trial was the basis to definitively evaluate this treatment approach and clinical outcomes in a larger clinical trial. KEYNOTE-689, which he helped design, is an international Phase 3 trial testing neoadjuvant/adjuvant pembrolizumab in resectable SCCHN patients.
Neoadjuvant Nivolumab Targets Oral Cavity Cancer
Dr. Uppaluri’s colleague, Jonathan D. Schoenfeld, MD, MPH, led the Phase 2 randomized clinical trial of neoadjuvant nivolumab or nivolumab plus ipilimumab in untreated oral cavity squamous cell carcinoma. Patients received either nivolumab only at weeks one and three, or nivolumab and ipilimumab at week one. Patients then had surgery three to seven days following the adjuvant treatment.
The treatments were well-tolerated, and promising response rates were observed with both treatment options. One-year progression-free survival was 85 percent, and overall survival was 89 percent.
“Importantly, we are finding that these neoadjuvant immunotherapy treatments don’t disrupt the standard of care or adversely affect surgical healing,” Dr. Uppaluri said. “If these therapies are approved for clinical practice after larger trials, they have the potential to allow for more limited surgery and de-intensified adjuvant therapy, thus reducing morbidity and improving clinical outcomes.
Moving the Needle on Patient Care
Dr. Uppaluri noted that the two Phase 2 clinical trials, along with current and future studies on adjuvant immunotherapy led by researchers at DF/BWCC, support the organization’s goal of constantly looking for ways to improve patient outcomes.
“We do standard of care very well,” he said. “But we’re always thinking about what we can do better to move the needle a little further, and our national leadership in neoadjuvant trials in surgical patients is one such way we are successfully doing this.”