Although there is no cure for pulmonary arterial hypertension (PAH), investigators from Brigham and Women’s Hospital are unraveling the molecular mechanisms that may control PAH’s development and progression in an effort toward finding treatments that could halt its advancement. In Science Translational Medicine, researchers shared results from a study that identifies the cancer protein NEDD9 as a critical player in disease development, with potential therapeutic implications for patients with PAH.
“Our work identifies a novel molecular target to prevent fibrosis in lung arteries, which can lead to early right-sided heart failure and death,” said corresponding author Bradley Maron, MD, a cardiologist, vascular biologist and PAH specialist at Brigham and Women’s Hospital. “Our data show that modification of proteins is an important mechanism that may account for the variability in fibrosis observed across human disease, with particular relevance to patients with PAH.”
“Accumulating evidence suggests that vascular fibrosis is one of the earliest events leading to remodeling of the pulmonary arteries, and therapeutic targeting of NEDD9 has the potential to stop further blood vessel damage and may prevent the right heart from failing,” added co-author Laura Fredenburgh, MD, of the Pulmonary and Critical Care Medicine Division. Fredenburgh also has investigated the role of the transcriptional regulators YAP and TAZ, which may trigger early pulmonary vascular fibrosis and may also be a potential new therapeutic target in PAH.
PAH is a severe form of cardiopulmonary disease in which the arteries that transport blood from the heart to the lungs become thickened, constricted and scarred. In PAH, fibrosis is an important cause of this damage, which increases strain on the heart and leads to perpetual shortness of breath. In the past, researchers had theorized that one pathway acted as a “master switch” to globally control fibrosis. But new evidence suggests that the development of fibrosis may be more complicated and more specific to different kinds of tissue.
To better understand which genes and proteins may influence scarring specifically in the lung arteries, Maron’s research team used network medicine – a method of mapping relationships between proteins, pathways and more. Through this approach, the researchers discovered that the cancer protein NEDD9 is a critical mediator of vascular fibrosis in lung blood vessels.
“There is a preconceived notion that increased fibrosis is pathological by definition. But the reality is that there are certain circumstances where fibrosis is an adaptive response to injury, suggesting that it is required for normal survival,” said Maron. “We used network medicine to refine the approach to understanding fibrosis, focusing on collagen function. We examined signaling pathways that are more specific to pathogenic fibrosis and then studied signaling pathways that are more specific for adaptive fibrosis.”
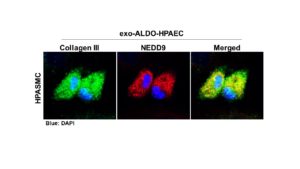
The researchers went on to identify a specific amino acid residue in NEDD9 that controls lung artery fibrosis. In patients with PAH, increased oxidant stress modifies this NEDD9 amino acid to cause lung artery fibrosis. The team also showed that the lung artery endothelium, previously regarded largely as a bystander in vascular fibrosis, contributes to this problem.
At the heart of the research team’s findings is NEDD9, which their data suggest mediates fibrotic vascular remodeling. The authors note that this has potential therapeutic relevance for PAH patients. A therapy that targets this protein has not yet been developed; but, because of its role in cancer, several studies have put NEDD9 forward as an important therapeutic target for future drug discovery efforts.
“The take-away is that the pulmonary circulation is vulnerable to injury, which can be studied on a molecular level, and one of the important hallmark features of that injury is vascular fibrosis,” said Dr. Maron. “Our work identified a novel pathway by which to explain vascular fibrosis in the context of pulmonary arterial hypertension. And this ultimately may have important implications for diagnosis, risk stratification and treatment of patients.”