Over a decade ago, Christopher Crum, MD, of Dana-Farber/Brigham and Women’s Cancer Center (DF/BWCC), helped design the protocol that revealed the fallopian tubes to be the origin of most high-grade serous carcinomas (HGSCs), the tumor type afflicting over two-thirds of women with ovarian cancer.
Now the pathologist is making progress in solving a paradox that has since vexed clinicians: Up to 90 percent of HGSCs are not detected until they are beyond the ovaries or fallopian tubes, at which point fully removing the tumor may not be possible. In contrast, only 30 to 40 percent of women who present with symptoms of advanced HGSC that has spread beyond the gynecological region show evidence of early cancer in the fallopian tubes.
“This is a fundamental mystery: Why do we catch the cancer so late even when we thought we were catching it early?” said Dr. Crum, recently the chief of the Division of Women’s and Perinatal Pathology at the Brigham.
For many years, it was mistakenly assumed that HGSC came from the ovaries. About two decades ago, however, surgeons began to identify early tumors in the fallopian tubes. In 2005, Dr. Crum conceived of the Sectioning and Extensively Examining the Fimbriated End Protocol (SEE-FIM) at the Brigham. Pathologists used this protocol to dissect the fallopian tubes, typically during prophylactic surgery to prevent cancer, and analyze them for signs of early cancers.
Results pointed to the distal fallopian tubes as the primary site for HGSC. SEE-FIM is now used in nearly every clinical laboratory in the country. The attention to the fallopian tube from this protocol has also led to the widespread adoption of opportunistic salpingectomy, which leaves the ovaries intact, for HGSC prevention.
Dr. Crum recently co-authored a paper published in The Journal of Pathology (Soong et al.) that shed more light on this topic. During an exhaustive analysis of seemingly “normal” fallopian tubes of 32 women with HGSC, very early signs of precancerous cells (which the investigators termed “early serous proliferations,” or ESPs) were found in 13 women. While ESPs are relatively common in the general population, most women who have them never develop ovarian cancer.
Suspecting that some ESPs might fuel the development of HGSC, the investigators sequenced TP53, a tumor suppressor gene that is mutated in all HGSCs. In 12 of the 13 women studied, the team detected a mutation in the ESPs that matched the mutation in the cancer found in the pelvis.
“In previous studies, we had learned there are multiple different types of mutations in the TP53 gene because there are so many different sites in the gene that can be mutated,” Dr. Crum explained. “So whenever you find two different pieces of the tumor that contain exactly the same site-specific mutation, the odds are they share the same cell of origin and are related.”
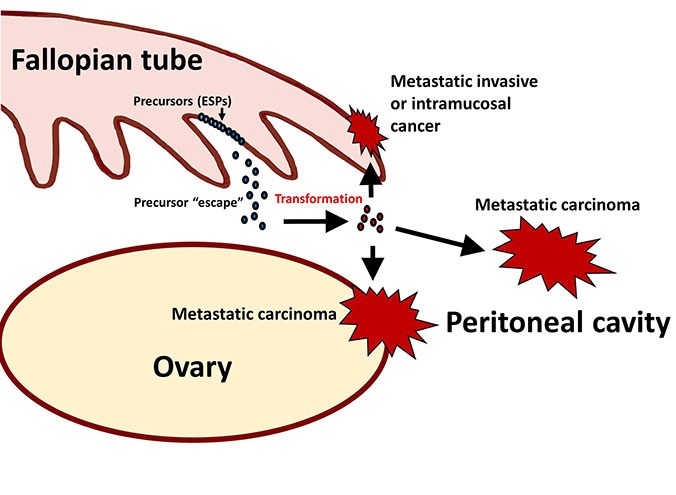
Based on these findings, the investigators concluded that some ESPs exit the fallopian tubes, eventually undergoing a malignant transformation in the peritoneal cavity and then spreading. They even coined a term for this phenomenon: precursor escape.
“The result is that the woman suddenly appears with widespread cancer, even though you don’t see any cancer in the fallopian tubes,” Dr. Crum said. “This is an important observation because it gives us new insights into how these tumors might develop, which had been a complete mystery. The notion that a few precancerous cells sitting in the tubes could ultimately be responsible for a malignancy out in the peritoneal cavity is a totally new concept.”
The question of why some ESPs become malignant remains unanswered for now. But the concept of precursor escape, if validated, could have important implications for HGSC prevention.
“Understanding more and more about where HGSC actually comes from puts you in a position to devise ways to prevent it,” Dr. Crum said. “I think this study gives us more confidence that the fallopian tubes are the source and the place to address through prevention. And that further strengthens the case for opportunistic salpingectomy in all women, especially high-risk women, when possible.”