Along with inflammatory arthritis, overproduction of autoantibodies is a defining feature of rheumatoid arthritis (RA), particularly autoantibodies against citrullinated proteins (ACPAs). The clinical significance of these ACPAs, other than for diagnosing RA, has been unclear. Previous studies have focused on association studies between a few ACPAs and one or two specific RA phenotypes – for example, an association between anti–citrullinated histone H2B antibodies and coronary artery calcium scores in patients with RA. But such an approach cannot identify potential associations with a wider array of untested phenotypes.
In a recently published article (Arthritis Rheumatology, 2017 Apr; 69(4): 742–749), Katherine Liao, MD, and colleagues applied the Phenome Wide Association Study (PheWAS) approach to screen for associations between ACPAs and potential subphenotypes of RA.
A PheWAS can be viewed as a Genome-Wide Association Study (GWAS) turned on its head. In a standard GWAS, an investigator tests for association between approximately one million genetic variants and one phenotype outcome, such as RA, yes or no. Using a standard PheWAS, it is possible to test for associations between genetic variants and a broad range of phenotypes.
The PheWAS generates a broad range of testable hypotheses and can be applied in large biobanks linked with electronic medical record (EMR) data. A published mapping converts groups of ICD9 codes into phenotypes. For example, RA would be defined as ICD9 714.x – ‘Rheumatoid arthritis and other inflammatory polyarthropathies. It was believed that the PheWAS could be an effective approach to examine whether the ACPAs differentiate RA into clinically relevant subgroups. Because the PheWAS was designed for genetic data, our interdisciplinary team of biostatisticians and bioinformaticians developed new methods that allowed screening for associations between groups of biomarkers – ACPAs – and multiple phenotypes.
This study was conducted in an RA cohort created using EMR data and linked to specimen samples that were measured for 36 autoantibodies with a published multi-bead assay. The autoantibodies were then grouped by their target protein for instance, the 10 antibodies against fibrinogen comprised one group. ICD9 codes for all RA subjects were then extracted and grouped into phenotypes using published PheWAS grouping methods.
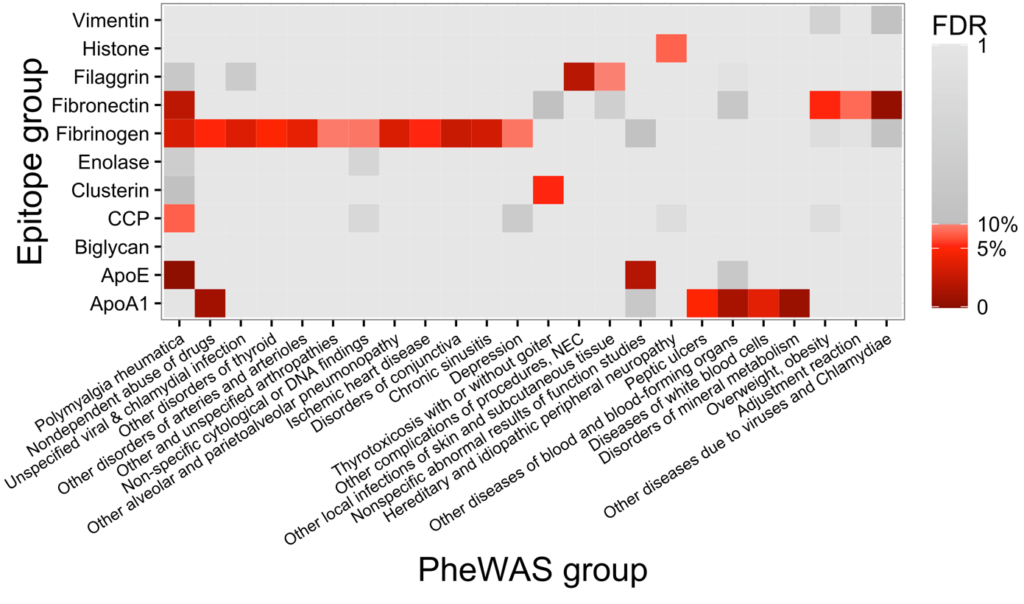
The analysis included 1,006 RA patients, 10 groups of autoantibodies, and 625 phenotypes, and identified an association between anti-citrullinated fibrinogen with ischemic heart disease, which confirmed- an earlier study that observed an association between anti-cit-fibrinogen and atherosclerotic plaque burden (see figure). Additionally, a strong association between autoantibodies against fibrinogen with inflammatory lung conditions was identified. Some of the strong associations found in this study are under investigation in prospective studies as potential biomarkers of risk for outcomes in coronary artery disease and interstitial lung disease among RA patients.